About Clinic
"Mending your broken pieces, keeps you moving"
Al-Ahli Hospital's Orthopedic & Traumatology Department benefits from a team of western trained, highly experienced Consultant Orthopedic and Spine Surgeons who are supported by a Team of experienced and well trained allied professionals. We are able to provide a complete orthopedic service to the adults and children we treat, through collaboration with all other departments within the hospital and particularly Physiotherapy, Radiology, Rheumatology, Neurology, Chiropractor and the Emergency Department.
The Orthopedic and Traumatology Department commenced its full time services in January 2009. The Department has grown rapidly since then with our team of Orthopedic Doctors increasing to 6 and appointment numbers increasing from 100 appointments per month in 2010 to 2,000 appointments per month in 2013.
The principles of the Orthopedic Department are simple:-
- Education and experience combined to ensure the staff of the Orthopedic Department are well equipped to assist our Guests on a day-to-day basis.
- Team work and a team of staff united in one common goal; striving to continually improve Guest service, Guest care and Guest satisfaction.
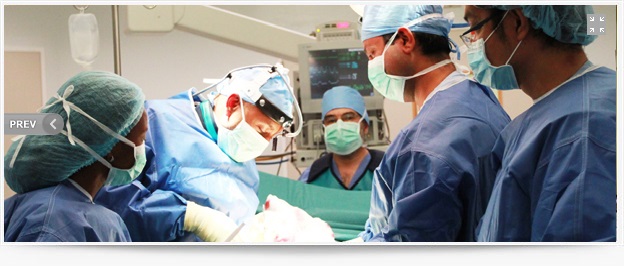
- Use of modern equipment and up-to-date minimally invasive surgical techniques to provide an extensive and fully inclusive service within the Orthopedic Department.
Each member of our Team is committed to providing a first class service to each and every one of our Guests and our goal for 2014 is to recreate the Orthopedic and Traumatology Department as a Centre of Excellence within Al-Ahli Hospital.